A cervical cone biopsy is a surgical procedure that extracts a cone or wedge-shaped piece of tissue from your cervix. If you have early stages of cervical cancer, your doctor will recommend the cervical cone biopsy procedure as a treatment, not a diagnostic tool.
Manhattan gynecology doctors offer comprehensive Obstetrics & Gynecology care for women of all ages. At our ob-gyn clinic, we provide a full range of gynecologic services, from annual check-ups and routine pap smears to performing LEEP’s, cervical cone biopsies, and GYN procedures. Our state-of-the-art OB/GYN facility in Midtown and the Upper East Side has the latest technologies.
Cervical Cone Biopsy
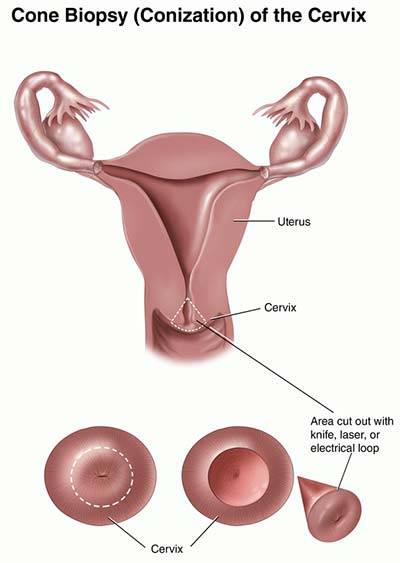 Your cervix is the opening between your vaginal vault and your uterus, also called your womb. Your cervix can open and close to protect your uterus. If your doctor suspects an abnormal condition, including cancer, collecting a biopsy or tissue sample may be the next step in your cervix. But standard biopsy procedures yield a small number of cells. When a more significant number is required, a cervical cone biopsy — also called conization — can help.
Your cervix is the opening between your vaginal vault and your uterus, also called your womb. Your cervix can open and close to protect your uterus. If your doctor suspects an abnormal condition, including cancer, collecting a biopsy or tissue sample may be the next step in your cervix. But standard biopsy procedures yield a small number of cells. When a more significant number is required, a cervical cone biopsy — also called conization — can help.
A cervical cone biopsy is a surgical procedure that extracts a cone or wedge-shaped piece of tissue from your cervix. Your doctor will send the removed tissue to the lab to check and analyze it under a microscope.
The size of the tissue sample required is a deciding factor when considering cervical cone biopsy vs. LEEP. This procedure captures a relatively large tissue sample. If your OBGYN only needs a small one, a LEEP suffices.
Why Do You Need a Cervical Cone Biopsy?
The procedure captures a tissue sample from your cervix.
The reasons your doctor might perform this operation include:
- Your Pap smear test results were abnormal, and you can’t be diagnosed with a minor biopsy.
- Your OBGYN suspects you have dysplasia (or enlargement) of the cervix or cervical canal.
- Your doctor has confirmed the early stages of cancer, such as adenocarcinoma in situ, on your cervix and can remove the cancerous cells to save your uterus.
- You have a human papillomavirus (HPV) infection on your cervix and need an HPV biopsy.
If you have cervical cancer, the recommended treatment may be a hysterectomy.But if your doctor caught cancer early enough, they can save your uterus by excising the cancer cells from your cervix using this procedure. In this case, the cervical cone biopsy procedure is a treatment, not a diagnostic tool.
What To Expect From a Cervical Cone Biopsy?
You have to be unconscious for this procedure, so you’ll likely receive general anesthesia. Even though a cervical cone biopsy is an outpatient surgery, you’ll need someone else to drive you home after you recover enough for the hospital discharge.
After you’re under anesthesia, your gynecologist inserts a speculum to get access to your cervix. Depending on the location of the abnormal or cancerous cells, the doctor may have to mechanically or chemically open your cervix.
Your doctor uses a surgical knife or a laser knife to cut. Then a wedge or cone-shaped section of tissue is cut from your cervix. After extracting the tissue, your doctor stops the bleeding with a natural product that packs the wound, helping it heal. The specialist will then send the biopsy to the lab for analysis. The whole operation takes less than an hour, usually between 30 and 45 minutes.
Are There Any Risks From the Procedure?
 Like any surgery, the cervical cone biopsy procedure carries some risks. It is safe, so complications are rare, but you could suffer:
Like any surgery, the cervical cone biopsy procedure carries some risks. It is safe, so complications are rare, but you could suffer:
- An allergic reaction to the anesthesia
- Infection
- Excessive bleeding
- Scarring of your cervix
- Blood clots in your legs
- Chest pain and shortness of breath
Many factors contribute to this issue. Your future Pap smear test results may be trickier to read. Additionally, depending on how much of your cervix the specialist removes, you may find pregnancy after cone biopsy challenging to achieve. Even if you get pregnant, you’re at a greater risk for a miscarriage or premature baby.
Talk to New York gynecologist, about your concerns. Also, keep in mind that most women recover from a cervical cone biopsy without any side effects.
How Does Will My Recovery Process Look?
After surgery, you’ll have some time to recover under the watchful eyes of recovery room nurses. Once you’re drinking on your own, your IV is disconnected. If you have a catheter in place, your doctor will remove it before you leave. When you’re conscious and well enough, your doctor will discharge you so your friend or family member can drive you home, where you’ll spend the rest of your recovery.
The anesthesia may make you weak and tired that first day. You’ll feel some post-cervical biopsy pain and cramping for two to three days after your procedure. Your doctor gives you a prescription for pain medication, and as you wean yourself off of that, you can take acetaminophen (such as extra-strength Tylenol) as needed.
You need to wear a pad for the next two weeks, as you’ll have some vaginal discharge. It may be bloody, and it may contain dark spots. This vaginal discharge is from the natural packing used to stop your bleeding after the surgery.
It would be best if you got out of bed to walk every day. Our doctors recommend that you take deep breaths and cough every three hours while you’re awake, at least for the first day, to strengthen your lungs.
Are There Any Recovery Warnings?
Everyone heals at a different pace. Your recovery can depend on your physical condition and age, as well as the severity of the procedure.
Follow your gynecologist instructions and:
- Do not have sex after cervical biopsy for four whole weeks.
- Do not use tampons or douche for four weeks.
- Do not do any heavy lifting or strenuous exercise for two weeks.
- You can return to work after two or three days, depending on your job and how you feel.
- You can drive once you stop taking prescription pain medicine that makes you tired.
Your recovery should progress every day. Typically, you only need to return to your Manhattan OBGYN Center for a follow-up visit, but call us immediately if you experience:
- Worsening and severe pain in your vagina
- A fever with a temperature over 100.5 degrees Fahrenheit
- Vaginal bleeding that forces you to change pads more frequently than once an hour
- A foul-smelling vaginal discharge that may be green or yellow
What Will I Have as the Result?
The cone-shaped tissue sample taken from your cervix will go to the lab for analysis. If a specialist finds cancer in it, you may need further, more invasive tests. You may need a total hysterectomy, which removes your uterus and cervix. It’s also possible that the tests will come back cancer-free.
Your procedure may have removed the precancerous or cancerous cells from your cervix, allowing healthy cells to grow back. Every case is different. Talk to your OBGYN about your concerns before you agree to a cervical cone biopsy.
All symptoms/diagnoses should always be evaluated with a thorough consultation and examination for an accurate diagnosis and treatment plan to exclude any serious underlying condition. You should always discuss the cervical cone biopsy procedure, indications, options, risks, and benefits with your gynecologist.
How to Prepare for a Cervical Biopsy?
Firstly talk with your doctor about the medication you take. Some of them may increase the chance of bleeding. Your cervical biopsy should be scheduled a week after the last period. Also, the critical point is that you can’t use tampons, douches, or medical vaginal creams for 25 hours before your biopsy.
Of course, you shouldn’t have sex during this period and eat before the cervical biopsy. You can eat something before the procedure at least 8 hours before. It would be better to have a family member or a friend with you since anesthesia produces drowsiness, and it is best to have someone drive you home. Ask your doctor if you can take painkillers before the procedure. It is important to bring women’s pads with you because bleedings are possible.
Is Cervical Biopsy Painful?
A cervical biopsy is not a painful procedure; you will be under anesthesia. After it, you will have cramping and spotting. But if you have noticed pain, you shouldn’t neglect it and contact a doctor because it’s a sign of infection.
How Long Does It Take To Get Cervical Biopsy Results?
In most cases, a doctor will contact you independently, and the average waiting time for the results is one to two weeks.
Have questions about the Cervical Cone Biopsy procedure? Schedule an appointment with nationally recognized specialists. Visit Manhattan Women’s Health and Wellness center in Midtown and on the Upper East Side to experience the best OBGYN NYC has to offer.
Updated on Sep 23, 2023 by Manhattan Women’s Health and Wellness
Best-in-class
New York Gynecology Clinic
Manhattan Specialty Care in the Press

Call now to make an appointment with our highly rated Manhattan Gynecology doctors regarding your health. We look forward to seeing you!
book online now
(212) 378-9985
New York City Locations:
Manhattan Women's Health & Wellness (Upper East Side)
983 Park Ave, Ste 1D17
New York, NY 10028
(212) 389-1904
Manhattan Women's Health & Wellness (Midtown)
56 W 45th St, Ste 815
New York, NY 10010
(212) 677-7654
Manhattan Women's Health & Wellness (Union Square)
55 W 17th St, Ste 104
New York, NY 10011
(212) 378-9985