Our doctors, a highly regarded obstetrician-gynecologists, treat endometriosis on a regular basis and can quickly alleviate your discomfort. Endometriosis does not have to cause painful periods for the rest of your life or prevent you from becoming pregnant. An NYC gynecologist, will examine you and discuss your treatment options when you visit him.
Endometriosis
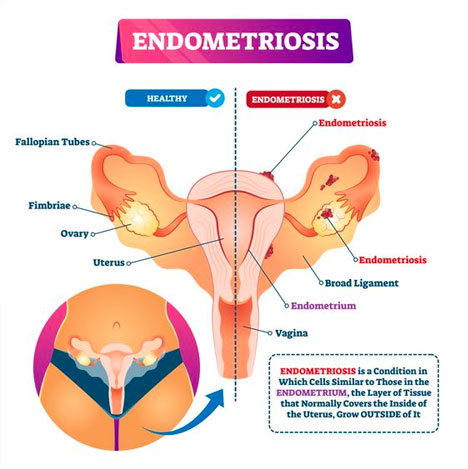
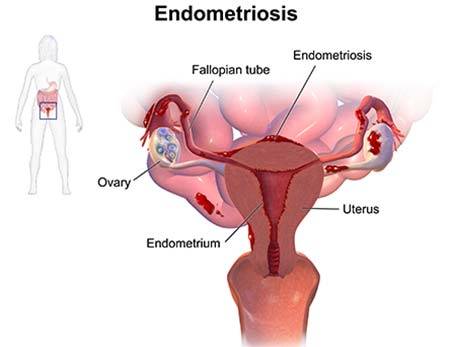 The endometrium is the tissue that lines the inside of your uterus. These tissues thicken, break down, and are expelled from your uterus each month as part of your menstrual cycle. When you have endometriosis, endometrial tissue implants outside the endometrial lining appear outside the uterus or on your ovaries, fallopian tubes, or pelvic lining.
The endometrium is the tissue that lines the inside of your uterus. These tissues thicken, break down, and are expelled from your uterus each month as part of your menstrual cycle. When you have endometriosis, endometrial tissue implants outside the endometrial lining appear outside the uterus or on your ovaries, fallopian tubes, or pelvic lining.
Your Midtown Manhattan gynecologist may find endometrial tissues in your vagina, cervix, or vulva. But they can also appear completely outside your reproductive system, in places such as your intestines, rectum, or bladder. They can even form, although rarely, in abdominal surgery scars. The endometrial tissue — regardless of its location and the fact that the tissue has no way to exit your body — continues its regular cycle of thickening, breaking down, and bleeding.
Signs and symptoms of endometriosis should always be evaluated with a thorough consultation and examination by a physician for an accurate diagnosis. A treatment plan can also follow up.
The Manhattan Women’s Health & Wellness offers comprehensive Obstetrics & Gynecology care in Manhattan for women of all ages. He provides a full range of gynecology services, from annual check-ups and routine pap smears to endometriosis treatment. Our state-of-the-art facility has the latest equipment.
Endometriosis Warning Signs
The initial signs of endometriosis are abnormally painful menstrual cramps that get worse over time. Endometriosis pain also can occur before you get your period or while having sex. However, while pain is the best-known symptom of endometriosis, you may not always recognize it.
Instead, other symptoms of endometriosis may present, such as:
- Fatigue
- Urination that’s painful during your menstrual cycle
- Bowel movements that are painful only during your period
- Other gastrointestinal issues, such as diarrhea, constipation, bloating, or nausea, especially during your period
- Heavy or excessive bleeding during your period and breakthrough bleeding from your uterus between your menstrual cycles
Because so many different diagnoses may include pelvic pain as a symptom, endometriosis can be hard to differentiate initially from diagnoses such as pelvic inflammatory disease, ovarian cysts, or irritable bowel syndrome.
It’s important not to let pelvic pain go unchecked. See the gynecologist or your local doctor for evaluation. Some women don’t discover they have endometriosis until they seek assistance in getting pregnant.
Certain factors may also put you at higher risk for endometriosis, such as:
- If you’ve never given birth
- If your period started at a younger than usual age
- If menopause started later than usual
- If your menstrual cycle is less than the standard 28 days
- If your body produces higher levels of estrogen
- If you have a low body mass index or BMI
- If you consume alcohol
- If you have one or more relatives who have been diagnosed with endometriosis
- If you’ve already been diagnosed with a medical condition that disrupts your menstrual cycle
- If you have any uterine abnormalities
- If you are Caucasian
Diagnosing Endometriosis
As with all female reproductive issues, the doctor first performs a pelvic exam. The best way to be sure of a correct diagnosis is to order a test so the Midtown gynecologist can better see what’s happening with your reproductive organs.
Unlike other diagnoses that may need several tests to be sure, the specialist can generally confirm endometriosis using only two tests:
- Ultrasound can be done in the office and helps identify cysts that may form from endometriosis. Growths like cysts or tumors show up on the image, although the test won’t show endometriosis definitively.
- Laparoscopy for endometriosis is a common procedure used to get a better picture of your organs. This test is the only one that shows whether you have endometriosis. For this test, your doctor puts you under general anesthesia, makes a small incision in your abdomen, and inserts a small scope with a light (a laparoscope). With it, women’s health professionals can examine the exterior of your uterus to discover any endometriosis and its extent. A biopsy may be taken at this time, especially if there are tissues that look suspicious in any way.
Steps After Diagnosis
Once you’ve been diagnosed with endometriosis, your doctor will explain the stages of the condition, which depend on several factors:
-
- How far and deep the endometrial tissues have spread
- If you have any fallopian tube blockages as a result
- The presence and severity of pelvic adhesions
Your case will fall into one of four endometriosis stages:
- Stage 1: Minimal
- Stage 2: Mild
- Stage 3: Moderate
- Stage 4: Severe
Which stage of endometriosis you fall into relates directly to your physical factors: the presence of adhesions or cysts, how many, how deep or severe, and so on.
Complications of Endometriosis
- Endometriosis cyst
- Infertility
- Ovarian cancer
- Pain
- Blood loss
Endometriosis Treatment in NYC (Midtown & Upper East Side)
Different treatments exist for endometriosis, depending on what stage you’re in and what your pain levels are. As a general rule, surgery is a last resort; your doctor will tailor your treatment to fit your lifestyle and needs. Your women’s health professional should perform diagnosis and treatment plans.
- Hormonal contraceptives and progestin therapy lighten your period.
- Estrogen-lowering hormones like the gonadotropin-releasing hormone (Gn-RH) agonists and antagonists are a great option. You may also use some newer similar medications like Orlissa.
- Danazol is a drug that blocks menstruation.
- The endometriosis diet is not a standard treatment yet, but studies have shown that women who eat a diet low in red meat and high in fruits and vegetables lower their chance of getting endometriosis.
- Physical activity can help with several estrogen-dependent conditions, including fibroids, menopause, and painful periods.
- If nothing else works, your local doctor may encourage you to get a complete hysterectomy to relieve your years of painful symptoms. The hysterectomy must be complete — that is, it must include the uterus, ovaries, fallopian tubes, and cervix — to remove estrogen-producing organs. Endometriosis after hysterectomy is no longer possible, and there’s total relief of symptoms.
Endometriosis and infertility are often linked. Women who have failed to get pregnant often discover their endometriosis when going for fertility treatments. Patients already diagnosed who now want to avoid surgery but still try to get pregnant can be directed to infertility treatments such as in vitro fertilization.
Endometriosis doesn’t have to mean painful periods for the rest of your life, nor does it mean you can’t become pregnant. While pregnant, endometriosis meets a temporary end and a permanent one with the onset of menopause.
Do you have any concerns about Endometriosis treatment? Make an appointment with Manhattan’s best gynecologist, today.
Updated on Sep 23, 2023 by Manhattan Women’s Health and Wellness
Best-in-class
New York Gynecology Clinic
Manhattan Specialty Care in the Press

Call now to make an appointment with our highly rated Manhattan Gynecology doctors regarding your health. We look forward to seeing you!
book online now
(212) 378-9985
New York City Locations:
Manhattan Women's Health & Wellness (Upper East Side)
983 Park Ave, Ste 1D17
New York, NY 10028
(212) 389-1904
Manhattan Women's Health & Wellness (Midtown)
56 W 45th St, Ste 815
New York, NY 10010
(212) 677-7654
Manhattan Women's Health & Wellness (Union Square)
55 W 17th St, Ste 104
New York, NY 10011
(212) 378-9985