Endometrial Polyps
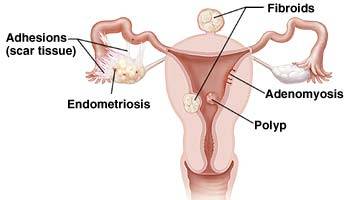 Endometrial polyps, also known as uterine polyps, are abnormal growths in your endometrium, the lining of your uterus. Excessive growth leads to the formation of polyps. Uterine polyps commonly occur in women who’ve undergone menopause, although younger women can get them too. You can have just one polyp or many.
Endometrial polyps, also known as uterine polyps, are abnormal growths in your endometrium, the lining of your uterus. Excessive growth leads to the formation of polyps. Uterine polyps commonly occur in women who’ve undergone menopause, although younger women can get them too. You can have just one polyp or many.
Endometrial polyps are attached to the inner wall of your uterus by a thin base or a stalk that connects them to the endometrial lining. Polyps can range in size and shape, from the size of seed all the way up to the size of a ping-pong ball.
Endometrial polyps irritate the surrounding tissues in your uterus and can cause pain or abnormal bleeding. Most endometrial polyps are benign or noncancerous. However, a small number can be cancerous or precancerous, which is why you must have them removed and sent to a lab to be analyzed. Your gynecologist should evaluate endometrial polyps with a thorough consultation and examination to determine an accurate diagnosis and treatment plan. It may be a symptom or sign of a severe illness or condition.
Our doctors specialize in polyps and their removal. Our clinic provides a full range of gynecology services, from annual check-ups and routine pap smears to Endometrial Polyps treatment and GYN procedures. At our state-of-the-art
Women’s Health Center, we have the latest OBGYN equipment.
Checking for Polyps
It’s not unusual to be unaware of uterine polyps; not everyone has symptoms. The most common symptom is unusual or spotty bleeding.
With bleeding polyps, you might see:
- Periods that last longer than they should
- Breakthrough bleeding or bleeding when you’re not on your period
- A heavier than normal or excessively heavy flow during your period
- Post-menopausal bleeding
- An inability to get pregnant or infertility
- Spotting
- Pelvic pain or painful periods
Any of these symptoms, especially if you notice them regularly, signal that something can be wrong. Please bring them to your doctor’s attention because the sooner you undergo the uterine polyps exam, the quicker your OBGYN can rule out more serious concerns. Your gynecologist can remove the polyps to reduce the abnormal bleeding you’re experiencing.
Causes and Risk Factors
 The exact cause of uterine polyps isn’t known, although studies show that hormones impact the formation of polyps, which grow in estrogen-rich areas. Additionally, polyps often appear where the endometrial lining has become overgrown.
The exact cause of uterine polyps isn’t known, although studies show that hormones impact the formation of polyps, which grow in estrogen-rich areas. Additionally, polyps often appear where the endometrial lining has become overgrown.
While causes are not concrete, doctors have identified several possible risk factors, such as if you’re:
- Overweight
- On cancer drugs such as Tamoxifen
- Perimenopausal or postmenopausal
- Have a personal history of endometrial or cervical polyps
Testing for Polyps
Since polyps show so few symptoms, the best way to diagnose and treat polyps is for gynecologist Midtown to order some tests. Many of these tests require mild sedation or localized anesthesia. All are minimally invasive procedures that leave no scars and require only about 24 hours for recovery.
- Sonohysterography, also known as hysterosonography, uses a tube to push sterile saline into your uterus to clarify the images made by a sonogram machine. Your doctor uses this test to see if there are any polyps or masses in your uterus. There should be minimal discomfort with this test, although some women do experience period-like cramping afterward.
The best time to schedule this test is seven to 10 days after your period ends. It would help if you weren’t on your period or pregnant during this test. For a few days following the test, the used fluids will seep out of your vagina throughout the day. Some of it may look a little bloody, but that’s normal.
- Endometrial biopsy is the removal of a tiny tissue sample from your endometrium. Your doctor will scrape out the endometrial biopsy polyp and then send it for analysis to rule out cancer. It may be required if you are over 35 and have abnormal uterine bleeding or are at a higher risk of cancer due to a family history of uterine cancer.
This procedure may cause some cramping during the test and discharge with small amounts of bleeding after the test. Post-procedure bleeding and cramping are not unusual. Mild pain relievers such as ibuprofen (Motrin) or acetaminophen (Tylenol) that don’t promote bleeding help you get through the discomfort.
- Hysteroscopy is a procedure that allows the doctor to see inside your uterus by using a tiny camera while you comfortably sleep.
- A basic pelvic exam may allow your doctor to find polyps, especially if you find a polyp on the cervix.
- Pap smear, a regular and routine test, may reveal abnormal cells if you have polyps.
- Ultrasound is another test that can detect masses in your uterus. It uses images made through sound waves from the outside by rubbing a wand over your abdominal area. This test allows your local OBGYN to check for ovarian abnormalities in addition to uterine polyps.
- Transvaginal Ultrasound is similar to an ultrasound. This test involves checking your vagina inside. It uses a vagina probe and not a wand on the outside of your abdomen.
- Dilation and curettage (D&C) are where your doctor gently cleans your uterine walls to obtain endometrium samples. At this time, it’s possible to detect a polyp on the cervix or polyps in the vagina.
- Hysterosalpingogram (HSG) is a procedure that uses dye injected into your uterus. X-rays reveal if there are any polyps.
Polyps sometimes come back, and they can occur more frequently in people who have had polyps in the past and have removed them. It is essential to visit your gynecologist regularly, especially if you develop any of the signs or symptoms of polyps.
Further Steps
Sometimes, you may not have to do anything if your polyps are tiny and cause no symptoms, but this is to be decided by your physician. It’s not unusual for polyps to resolve independently, where your body re-absorbs them without incident. However, if they aren’t shrinking on their own or become pre-cancerous or cancerous, gynecologist will have to take measures.
Further steps may include:
- Some medications containing hormones, such as progesterone and gonadotropin-releasing hormone agonists, might help you with any symptoms you’re experiencing with polyps. Typically, once you stop taking these drugs, the polyps return. The medications mentioned above may be the best treatment if you have endometrial hyperplasia, an overgrowth of the cells in the endometrium.
- ften, surgery is the last resort. If your gynecologist Midtown has ordered a hysteroscopy as a test, removing the polyps found may be performed as part of this minimally invasive procedure. Your doctor will send anything removed during this test to a lab, just as with a biopsy. If the polyps turn out to be precancerous or cancerous, then your OBGYN in NYC will most certainly order them all removed and carefully followed by your physician.
Have questions about Endometrial Polyps? Please schedule an appointment with the top New York City Gynecologist by contacting our office today.
Updated on Sep 23, 2023 by Manhattan Women’s Health and Wellness
Best-in-class
New York Gynecology Clinic
Manhattan Specialty Care in the Press

Call now to make an appointment with our highly rated Manhattan Gynecology doctors regarding your health. We look forward to seeing you!
book online now
(212) 378-9985
New York City Locations:
Manhattan Women's Health & Wellness (Upper East Side)
983 Park Ave, Ste 1D17
New York, NY 10028
(212) 389-1904
Manhattan Women's Health & Wellness (Midtown)
56 W 45th St, Ste 815
New York, NY 10010
(212) 677-7654
Manhattan Women's Health & Wellness (Union Square)
55 W 17th St, Ste 104
New York, NY 10011
(212) 378-9985