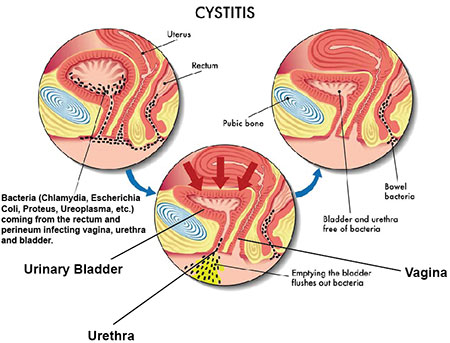
 Cystitis refers to the medical condition when your bladder is inflamed, swollen and tender, or more simply put, a urinary tract infection (UTI).
Cystitis refers to the medical condition when your bladder is inflamed, swollen and tender, or more simply put, a urinary tract infection (UTI).
If you have an infected bladder, you may experience other symptoms besides pain in your lower abdomen, such as:
- Discomfort or uncomfortable pressure in your bladder
- A constant need to urinate, but you’re only able to urinate a little bit each time
- A painful burning when you urinate
- Blood in your urine
- Translucent and concentrated (smelly) urine
- Cloudy or murky urine
- Possible fever
Cystitis is a treatable condition. It would be best if you visited your gynecologist or OBGYN specialists because untreated cystitis (UTI) can lead to a worse problem that may require hospitalization. Besides suffering from increasingly worse symptoms, the infection can spread to your kidneys, where it’s more challenging to treat.
If you experience any of the following symptoms of an infected kidney, seek medical attention:
- Pain from the area of your kidneys, which are in the back of your upper abdomen
- Fever
- Feeling nauseous or even vomiting
All symptoms should be evaluated with a thorough consultation and examination by your gynecologist for an accurate diagnosis and treatment plan to exclude any serious underlying condition.
Gynecologists of Manhattan Women’s Health & Wellness offer comprehensive NYC Obstetrics & Gynecology care for women of all ages. At our OBGYNclinic, we provide a full range of gynecology services, from annual check-ups and routine pap smears to Bladder Infection treatment and GYN procedures, surgeries performed in our office or the hospital. Our state-of-the-art gynecology facility in NYC has the latest OBGYN equipment.
What Causes Cystitis
Often, the cause of cystitis is a bacterial infection — a urinary tract infection or UTI — that reaches your bladder. UTIs are common in women since your vagina naturally contains various bacteria. Besides, the little pipe (urethra) that connects the bladder to the outside world is much shorter than males. Sexual intercourse, therefore, sometimes causes a UTI. But obviously, that’s not the only way to get a UTI since women who aren’t sexually inactive still can suffer from an infected urinary tract. Bacteria can migrate from the rectum to the urethra and then to the bladder.
The pain and inflammation of cystitis can result from several other conditions as well, although these causes are less common:
- Continual use of irritation-causing products, such as chemical-based feminine hygiene products and contraceptives
- An allergic reaction to some feminine hygiene products, contraceptives, or even bubble bath
- As a reaction to certain medications, especially chemotherapy drugs
- Using a catheter for a long time
- Chronic inflammation of your bladder (Interstitial Cystitis)
- From radiation therapy to treat cancer
- Other medical conditions — such as kidney stones or diabetes — can cause cystitis as a complication.
Weighing Your Risks
Cystitis can strike any woman, but there are some things you can do to reduce your risk of getting a urinary tract infection. Since a UTI is one of the primary causes of cystitis, reducing your chances of getting one also reduces your susceptibility to cystitis. At the same time, some risk factors are purely physical, such as having a shorter urethra, which shortens the distance bacteria has to go to get to your bladder.
The best advice is to be aware of when you might be suffering from a UTI so you can treat it promptly.
Here are other risk factors for developing a UTI:
- Being sexually active
- Using some contraceptives, such as some vaginal rings and spermicidal creams
- Experiencing a bladder stone or a kidney stone
- Being pregnant
- Being postmenopausal
- Having other medical conditions like diabetes or cancer
- Using a catheter over an extended period
- Getting cancer treatments, including radiation and chemotherapy
Untreated or incomplete UTI treatment can allow the bacteria to infect the kidneys, which can be a life-threatening situation.
Testing for and Treating Cystitis
Since cystitis symptoms can also indicate other, more serious medical conditions like ovarian cysts, it’s essential to see your gynecologist if you’re experiencing any of the symptoms listed above. Your OBGYN can usually rule out other conditions to arrive at an accurate diagnosis. Then your treatment can begin.
The Cystitis tests gynecologist may order include:
- A urine analysis, which can detect the presence of blood, bacteria, or other foreign matter in your urine
- A cystoscopy, for which your NYC OBGYN inserts a thin tube with a light and camera on end, called a cystoscope, into your urethra to look for telltale signs of disease or infection.
- An X-ray or ultrasound test (such as a sonogram) can produce a better picture of what’s going on with your bladder — especially when other tests fail to provide any clues.
Once your doctor has confirmed a diagnosis of cystitis, the most common treatment is to put you on a course of antibiotics. The antibiotic and the length of time you have to take it depend on your medical history, allergies, the type of bacteria, and the severity of your infection. The usual course is three to seven days, with a follow-up exam to ensure the problem has completely disappeared.
If you’ve been suffering from several UTI’s a year, tell your OBGYN. You may need different treatment or at least a different type of antibiotic. It’s also possible that your cystitis occurred due to an underlying cause that you cannot treat by antibiotics. In this case, your gynecologist may have to run additional tests to find that underlying cause so the doctor can treat it effectively.
Complications Associated with Cystitis
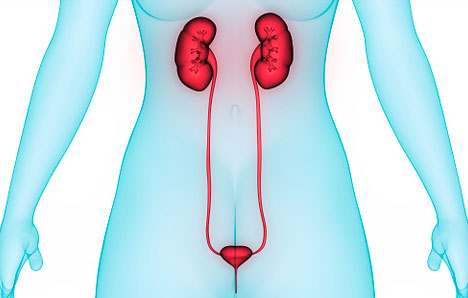 The most severe complication from cystitis — and the main reason to treat it right away — is the danger of kidney infection. Pyelonephritis, a kidney infection, can permanently injure your kidneys. The longer the condition goes untreated, the worse it can become.
The most severe complication from cystitis — and the main reason to treat it right away — is the danger of kidney infection. Pyelonephritis, a kidney infection, can permanently injure your kidneys. The longer the condition goes untreated, the worse it can become.
Sometimes, you’ll have blood in your urine that’s not visible to the naked eye. A urine analysis test, however, can spot the blood. If this condition continues even after your antibiotic treatment, you may need to undergo further testing to determine the cause of the blood in your urine.
If you get cystitis during a hospital stay, the chances are that the bacteria causing your UTI are resistant to the most common types of antibiotics. Treating cystitis in a hospital usually means a more aggressive therapy or more potent antibiotics, which sometimes have unintended side effects. Fortunately, infections from a hospital stay are on the decline, although catheter-related infections have stayed the same since 2009.
When to Call Your NYC OBGYN
Your gynecologist should evaluate symptoms with a thorough consultation and examination for an accurate diagnosis and treatment plan to exclude any severe or underlying condition. If your symptoms return after you’ve finished your antibiotics, call or return to Manhattan gynecologist for a consultation and exam. You may need a different antibiotic, or the renewed symptoms could signal a more serious problem.
Have questions about Pelvic Pain, Cystitis, or Bladder Infection? Schedule an appointment with one of the best-rated NYC Gynecologist today.
Updated on Sep 23, 2023 by Manhattan Women’s Health and Wellness
Best-in-class
New York Gynecology Clinic
Manhattan Specialty Care in the Press

Call now to make an appointment with our highly rated Manhattan Gynecology doctors regarding your health. We look forward to seeing you!
book online now
(212) 378-9985
New York City Locations:
Manhattan Women's Health & Wellness (Upper East Side)
983 Park Ave, Ste 1D17
New York, NY 10028
(212) 389-1904
Manhattan Women's Health & Wellness (Midtown)
56 W 45th St, Ste 815
New York, NY 10010
(212) 677-7654
Manhattan Women's Health & Wellness (Union Square)
55 W 17th St, Ste 104
New York, NY 10011
(212) 378-9985